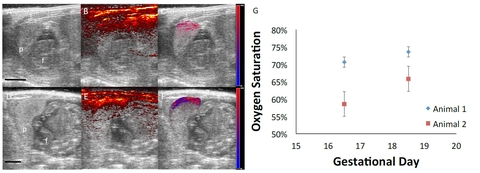
Figure 1: Ultrasound-guided photoacoustic imaging of rat placental oxygenation. (A,D) Ultrasound images of fetal anatomy at gestational day 16.5 (A) and day 18.5 (D) of normal pregnancy. (B,E) PA signal overlaid on the ultrasound shows strong attenuation within the skin and placenta due to the presence of oxy- and deoxyhemoglobin. (C,F) Oxygen saturation in the placenta. Red denotes completely oxygenated blood and blue represents deoxygenated blood. Scale bars = 5mm. (G) Mean and standard deviations of oxygen saturation in the placenta (5 placentas per animal, 2 animals).
Submitted by Dr. Carolyn Bayer from Tulane University in New Orleans, LA.
There is an urgent need to identify first trimester pregnancies at risk for the development of preeclampsia—a leading cause of maternal and perinatal mortality—in order to improve clinical treatment of the disease. Preeclampsia is thought to initiate with placental ischemia—reduced blood flow to the placenta—which may result from inadequate placental development and invasion. Placental ischemia causes the release of factors, leading to the clinical symptoms of preeclampsia—high blood pressure and proteinuria. There are no clinically-approved methods to treat placental ischemia or preeclampsia; the only “cure” is the premature delivery of the placenta and fetus. Using the reduced uterine perfusion pressure (RUPP) rat model to examine the biomolecular pathways leading to the development of preeclampsia, researchers have identified potential therapeutic targets for clinical translation. Our research laboratory is developing ultrasound-guided spectral photoacoustic imaging of placental ischemia in vivo.
Ultrasound imaging and its variants are preferred for prenatal imaging due to its relative safety and low cost. Ultrasound imaging generates high resolution, real-time images of the maternal and fetal anatomy, while Doppler ultrasound produces measures of uterine artery and umbilical blood flow. Photoacoustic imaging — using nanosecond light pulses to generate ultrasound signals — provides high contrast images of hemoglobin in blood. By varying the wavelength of the incident light and recording the photoacoustic signal strength — termed spectral photoacoustic imaging — we are able to produce regional tissue maps of hemoglobin oxygen saturation.
We are developing our placental ischemia imaging methods using the RUPP model of placental ischemia and preeclampsia. The RUPP rat is ideal for the development and validation of our imaging methods, since the technique physically modifies the blood flow to the placenta — rather than relying on an indirect chemical method — providing improved reproducibility. In our preliminary studies, levels of placental oxygenation were measured in Sprague-Dawley timed pregnant rats. We acquired images of 5 placentas per animal, at two developmental time points, using the Vevo 2100 system and a LZ250 transducer. The ultrasound, photoacoustic signal, and linear regression estimation of the oxygen saturation—segmented to the placenta—is shown in Figure 1.
Currently, we are implementing the RUPP surgical model and acquiring pilot data on longitudinal placental ischemia in this preclinical model of placental ischemia. We believe this work will provide insight into the importance and onset of placental ischemia in the development of preeclampsia and provide a model to test potential therapeutics. This pilot work was funded by a Tulane University Carol Lavin Bernick Faculty Grant.